Rukmini S
 The case fatality rate number for a country misses taking into account a host of factors that affect it – most crucially, age.
The case fatality rate number for a country misses taking into account a host of factors that affect it – most crucially, age.
New survey estimates are producing Covid-19 fatality rates for India that are lower than virtually anywhere else in the world by orders of magnitude. But the current narrative around these fatality rates could be doing a disservice to India’s understanding of the disease by being too quick to attribute them to the government’s “successful strategies” rather than searching for the underlying biological and sociological causes that could explain them, experts say.
The Indian government frequently reiterates that India’s Covid-19 mortality is particularly low compared to the rest of the world, and Prime Minister Narendra Modi has singled out this indicator for praise too.
This claim has mostly relied on a crude measure called the case fatality rate. It is simply the total number of reported Covid-19 deaths by a particular date divided by the number of Covid-19 cases confirmed by that date.
But a single headline case fatality rate number for a country misses taking into account a host of factors that affect that number – most crucially, age. All evidence up to this point has shown that the SARS-CoV-2 virus disproportionately affects the elderly.
Given that India is a relatively young country, this could drive down its case fatality rate, experts have suggested.
Yet, a number of studies have now shown that taking age into account, India’s age-adjusted case fatality rate is not particularly low.
In a recent National Bureau of Economic Research working paper, for instance, economists Minu Philip and Debraj Ray, and researcher S Subramanian find that India’s age-adjusted Covid-19 mortality rate is actually higher than would be expected if the age-specific case fatality rates of 14 countries – including some European, developed East Asian and Latin American countries – were applied to India. While India is substantially younger than these countries, its young population has also been disproportionately affected, their paper shows.
 “Among adult groups and relative to the comparison countries, India stands out in having a large impact ratio for all but the oldest ages,” they write. “These relatively young and middle-age groups are not only those excessively represented in the overall population, but they are also disproportionately more affected by Covid-19.”
“Among adult groups and relative to the comparison countries, India stands out in having a large impact ratio for all but the oldest ages,” they write. “These relatively young and middle-age groups are not only those excessively represented in the overall population, but they are also disproportionately more affected by Covid-19.”
As the pandemic progresses, many in the scientific and public health community are moving away from calculating case fatality rate based on recorded cases alone to considering the mortality from Covid-19 in the broader population. But once again, India is emerging as an outlier.
Across the world, serological surveys are allowing researchers to estimate the extent of SARS-CoV-2 antibody in the population, and from that the infection fatality rate. It is the total number of reported Covid-19 deaths by a particular date – so the same numerator as in the case fatality ratio – but divided by the estimated total number of infections in the population, whether already detected or not. (Researchers would use the extent of spread of the infection that sero-surveys show to estimate what the total number of detected and undetected cases in the population might be.)
In early July, the World Health Organization’s Chief Scientist Soumya Swaminathan placed this derived infection fatality rate for the world at somewhere in the range of 0.6%. Other global studies have found similarly; the United States’s Centre for Disease Control “current best estimate” (as of July 10) for the infection fatality rate is 0.65%. A meta-analysis of global estimates in early July estimated the infection fatality rate at 0.68%.
And then there are the Indian estimates.
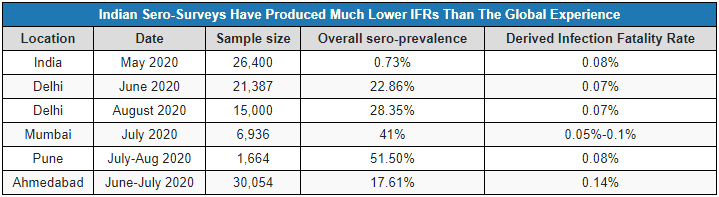 Since the beginning of July, sero-prevalence surveys have sprung up across the country. In June, the Indian Council of Medical Research first presented early findings from a pan-Indian sero-survey that split the country into four groups from 15 districts, going from low incidence based on what RT-PCR testing at the time was showing, to high incidence. That survey found a sero-prevalence of 0.73% and a derived infection fatality rate of 0.08%.
Since the beginning of July, sero-prevalence surveys have sprung up across the country. In June, the Indian Council of Medical Research first presented early findings from a pan-Indian sero-survey that split the country into four groups from 15 districts, going from low incidence based on what RT-PCR testing at the time was showing, to high incidence. That survey found a sero-prevalence of 0.73% and a derived infection fatality rate of 0.08%.
The National Centre for Disease Control conducted a similarly stratified sero-survey in Delhi from June 27 to July 1, which they said showed a sero-prevalence of 23% and a derived IFR of around 0.07%. The second round conducted by Maulana Azad Medical College in the first week of August found sero-prevalence had risen to 28%, producing a derived IFR of roughly the same value.
In Mumbai, the Tata Institute of Fundamental Research, Niti Aayog and the Municipal Corporation of Greater Mumbai collaborated on a sero-survey that was conducted in three wards of the city, one each of which was a low, moderate and high prevalence ward, based on what current RT-PCR testing was showing.
The sample was stratified by age and gender and was split into slums and non-slum housing. The researchers found that prevalence was at 51-58% in the slum areas of the three wards, and at 11-17% in the non-slum areas. This produced a derived infection fatality rate of 0.05% to 1%. A sero-survey in Pune found even higher sero-prevalence, which would imply an even lower derived infection fatality rate.
The levels of sero-prevalence demonstrated by the Delhi, Mumbai and Pune sero-surveys would imply infection fatality rates that are orders of magnitude lower than global estimates.
Even if there is significant under-counting of Covid-19 deaths in India, it will not materially alter these rates, Giridhar Babu, an epidemiologist at the Public Health Foundation of India, said in an interview to IndiaSpend.
Why India is producing such low infection fatality rates then is something that requires deep investigation, he said. But even before that, the agencies that have led the Indian surveys have been quick to attribute the unusually low infection fatality rate to “successful” measures undertaken by governments.
Presenting the preliminary findings of the ICMR’s first national sero-survey on June 11, Balram Bhargava, director-general of the ICMR, attributed the low sero-prevalence –under 1% at the time – to the government’s lockdown, and said, “The good news is that the infection fatality rate was very low.”
At the same press conference, VK Paul, who heads the Covid-19 response task force, said, “In such a big country, such a big pandemic was kept at this level by the country, this is in itself a very important achievement, there should be no doubt about that.”
“The mortality rate in this country on account of the pandemic is clearly low,” he added. “And this is also a matter of good fortune.”
By July, sero-prevalence was no longer low, but the infection fatality rate was, and the government’s policies were up for praise.
“This shows us one more thing that the aggressive lockdown measures or containment measures that were taken right from the beginning prevented this infection from taking a severe form,” said the Director of National Centre for Disease Control, Sujeet Kumar Singh, presenting their Delhi survey’s findings that they said showed 23% of the population had antibodies.“This points to the success of those measures.”
In a technical note accompanying the Mumbai survey published by TIFR, the authors say that the city’s low infection fatality rate could be attributed to “effective containment efforts and active measures to isolate symptomatic cases by MCGM [the municipal corporation].” Later, they suggest that “social distancing and related precautions such as wearing masks are effective in slowing the infection spread.”
Questions not raised, or answered
These claims do not answer one key question – If infections seem to have spread wider in India than almost anywhere in the world to produce sero-positivity levels seen in few other countries, what is so unusual about India that is keeping deaths so low? If the only explanatory variable was “successful containment measures”, surely South Korea should have done better?
The low derived infection fatality rate was not a result of over-estimation of sero-prevalence, but could have multiple other explanations, Singh, the National Centre for Disease Control director, told IndiaSpend.
“We have a very young population, so that could be one explanation,” he said. “Then another explanation is that our population could have some underlying immunity.”
Age as a complete explanation for India’s “low” mortality, however, is contentious, given India’s unusually high age-adjusted mortality for younger age groups.
The TIFR’s principal investigators for the study, scientists Ullas Kolthur-Seetharaman and Sandeep Juneja, suggested similar possible explanations in an interview with IndiaSpend.
Firstly, the age-adjusted infection fatality rate is not orders of magnitude lower in India, Juneja said.
“If you were to adjust for age, the infection fatality rate for Spain or even Wuhan would be around 0.2% and what we are seeing is 0.1%,” he said. Underlying immunity, he said, could potentially explain some of this gap.
“The infection fatality rate in our survey is actually lower for the slums and higher for the non-slums,” he said. “If you look at the non-slum areas, it’s actually very similar to what you would expect – it’s actually more than 0.2%. You could speculate why this is – the slum population could be younger, people in slums could have lower co-morbidities, and third could be that they’ve developed some immunity.”
While neither of these explanations has been shown to have a proven link yet to lower mortality, they could provide research directions.
There is now an emerging pathway to think about how this immunity could be studied. Priya Sampathkumar is Chair of Infection Control at the Mayo Clinic in Rochester, Minnesota, in the United States.
She recently put together a Twitter thread of emerging global evidence in a Twitter thread on cross-reactive immunity as suggested by the presence of T-cells (cells indicative of an immune response) reactive to Covid-19 present in persons seemingly without exposure to the virus.
“I think this could explain the lower mortality [in India],” she said in an interview to IndiaSpend. “Even if large numbers of people get infected, the illness is milder because of pre-existing cross immunity from past infection with other coronaviruses.”
Pursuing this hypothesis would require testing for T-cell related immunity, which Sampathkumar points out is much harder to measure than antibodies. Additionally, the presence of the cells does not guarantee that they are producing effective immunity in a person, and in India there is a particular concern – “Nutrition impacts T-cell immunity to a great extent.”
Whether India’s low infection fatality rate is a biological fact, or a product of its younger population is not yet established. Murad Banaji, a senior lecturer in mathematics at the University of Middlesex in London, looked at age-adjusted infection fatality rates and found that Mumbai’s age-adjusted infection fatality rate is, in fact, inexplicably high in the 40-60 age group.
What is, however, clear is that blanket praise for the government for ‘keeping’ the infection fatality rate low will not take India’s understanding of the pandemic very far.
“People are very quick to take at face value these low values of infection fatality rates that are coming up from sero-surveys without really attempting to unpack them and ask why,” Banaji said.
In the absence of any clear evidence yet that there is something materially different about India, much more work needs to be done to understand why this is happening, Babu said.
Courtesy Scroll.in






















































 The case fatality rate number for a country misses taking into account a host of factors that affect it – most crucially, age.
The case fatality rate number for a country misses taking into account a host of factors that affect it – most crucially, age.











